Matthew was discharged from the hospital last Friday night. By Saturday I noticed increased nausea and vomiting. The little voice in the back of my head told me I needed to call transplant, but my mind got the better of me. I knew we had been in the hospital the night before and chalked up his increase of symptoms to fatigue from his previous hospitalization. Sunday was a big day. Matt was getting back into town Sunday night from a conference he had attended the week before in Arizona. Joshua was being presented in sacrament meeting as a graduate from primary and was going to recite an article of faith and bear his testimony. I was also asked to go to primary on Josh's last day to talk about how "The faith in God" program was a blessing in our family. My great friend and visiting teacher, Kathryn Hart, agreed to come and sit with Matthew while I went to Primary but I just couldn't miss supporting Josh for sacrament meeting. I never feel good about asking somebody else to miss sacrament meeting so that I can attend- so I came up with a plan. Matthew was coming with me- I'd sneak in the very back and then leave right after the sacrament. It seemed to work, but when I got home I realized that the 20 minutes we were gone completely wore Matthew out. He perked up for Kathryn when I went to Primary to support Josh on his last day. When things settled down a bit I realized that Matthew was the same as he had been the day before. I paged the transplant coordinator who was on call on Sunday and she told me she thought we should come in first thing the next day to be seen.
On Monday morning we did bloodwork, an echo, and had a visit with Dr Tani. Based on Matthew's labs and his clinical findings Dr Tani felt Matthew's heart failure had gotten worse. Matthew's BNP went from 600 to 1500 in a matter of days. We were admitted to the CICU for an increase of Milrinone. Matthew is super fluid over loaded so they increased Lasix to three times a day and started Diuril and Aldactone to better dierese his extra fluid. Because his gut cannot even handle Neocate at a small rate through his G-tube (and he wasn't meeting his daily caloric needs anyway) they started TPN along with some additional lipids.
They decided to transfer Matthew out of the ICU tonight- so we are on the floor now. Matthew is technically on a dose of Milrinone that should keep him in the hospital to be monitored. To be honest, I feel like Matthew's care is over my head at this point. He is so sick already and his symptom changes indicating problems are so subtle that I'm afraid I'll miss something if he comes home.
Matt and I have an appointment with the CV surgeon, the transplant cardiologists, palliative care, the social worker, and GI to discuss the progression of his multi systems beginning to fail and the possibility of using an LVAD (left ventricular assist device) as a bridge to transplant. This meeting will take place next Wednesday when the transplant team gets back from a conference they've been attending this week. I'm not sure how Matt and I feel about the LVAD. The placement of this pump would require open heart surgery and a full time CICU stay until transplant which could take awhile still. I feel like things could get real ugly real quick and I'm scared!!
I'll keep you updated after we know more. As you know this whole process is a day by day process. Things change so quickly. Please pray for Matthew!!
Thursday, April 19, 2012
Subscribe to:
Post Comments (Atom)



We will keep Matthew and your family in our prayers. So much love comes thru your posts. What lucky little boys to have such a mommy (and daddy). Keep your chin up knowing so many people care about what's happening in your lives. Love you - Corinne
ReplyDeleteI'm always praying for Matthew and your family. My heart breaks when I hear what that sweet little guy has to go through to stay here with his family but my prayers are always asking Heveanly Father for more strength for Matthew and his loving family to make it to the next step in the right direction. I know we still haven't met in person but I feel as though we become connected as friends through our experiences and I hope you know that if you ever need anything I will be there for you.
ReplyDeleteLove
Amy Saville
Praying for you, your family, and especially Little Matthew. My heart sank the other night hearing of your visit to the CICU. I know that you and Matt will be blessed with the help of Heaven as you make decisions. Thinking of you ALWAYS. I wish I were there...
ReplyDeleteLove,
Teresa
PS Thank you so much for the update.
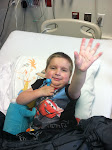
I just have to add, you are such INCREDIBLE parents. I tear up everytime I look at the picture of you with Matthew...SO much love.
ReplyDeletePraying you and Matthew everyday.
ReplyDeleteLove you guys so much! Give Matthew a big hug for us! As always, we are praying for you guys and sweet matthew! Matthew is blessed to have such amazing parents!
ReplyDeleteChrissy:
ReplyDeleteI am so sorry for all that Matthew and your family are going through. What a long and difficult road it has been. You are all in our prayers right now, especially sweet Matthew...what a trooper. Praying for good news soon!
Oh, this must be SO terribly hard. I can not even imagine how painful all this must be. I know you have such strong faith and are such a good mama! I am sure Matthew knows how much you love him and would give anything to take this from him. It all really is in the Lords hands, sometimes that must be so hard. I have been pondering this talk a lot lately and when I read your post, I immediately thought of you. I'll continue to be praying that you'll have the strength to bear your burdens. Love you!
ReplyDeletehttp://www.lds.org/general-conference/2012/04/mountains-to-climb?lang=eng
"If we have faith in Jesus Christ, the hardest as well as the easiest times in life can be a blessing. In all conditions, we can choose the right with the guidance of the Spirit. We have the gospel of Jesus Christ to shape and guide our lives if we choose it. And with prophets revealing to us our place in the plan of salvation, we can live with perfect hope and a feeling of peace. We never need to feel that we are alone or unloved in the Lord’s service because we never are. We can feel the love of God. The Savior has promised angels on our left and our right to bear us up.10 And He always keeps His word."